Quick Summary: Explore how computer vision is transforming healthcare, improving diagnostic accuracy, and optimizing workflows. Learn how to implement this technology, choose the right development partner, and overcome challenges. This blog offers actionable insights for healthcare professionals looking to enhance patient care and operational efficiency with AI-powered computer vision.
You read medical images every day, where a single missed detail can change the entire diagnosis. X-rays, CT scans, pathology slides, and retinal images demand consistent precision across every case.
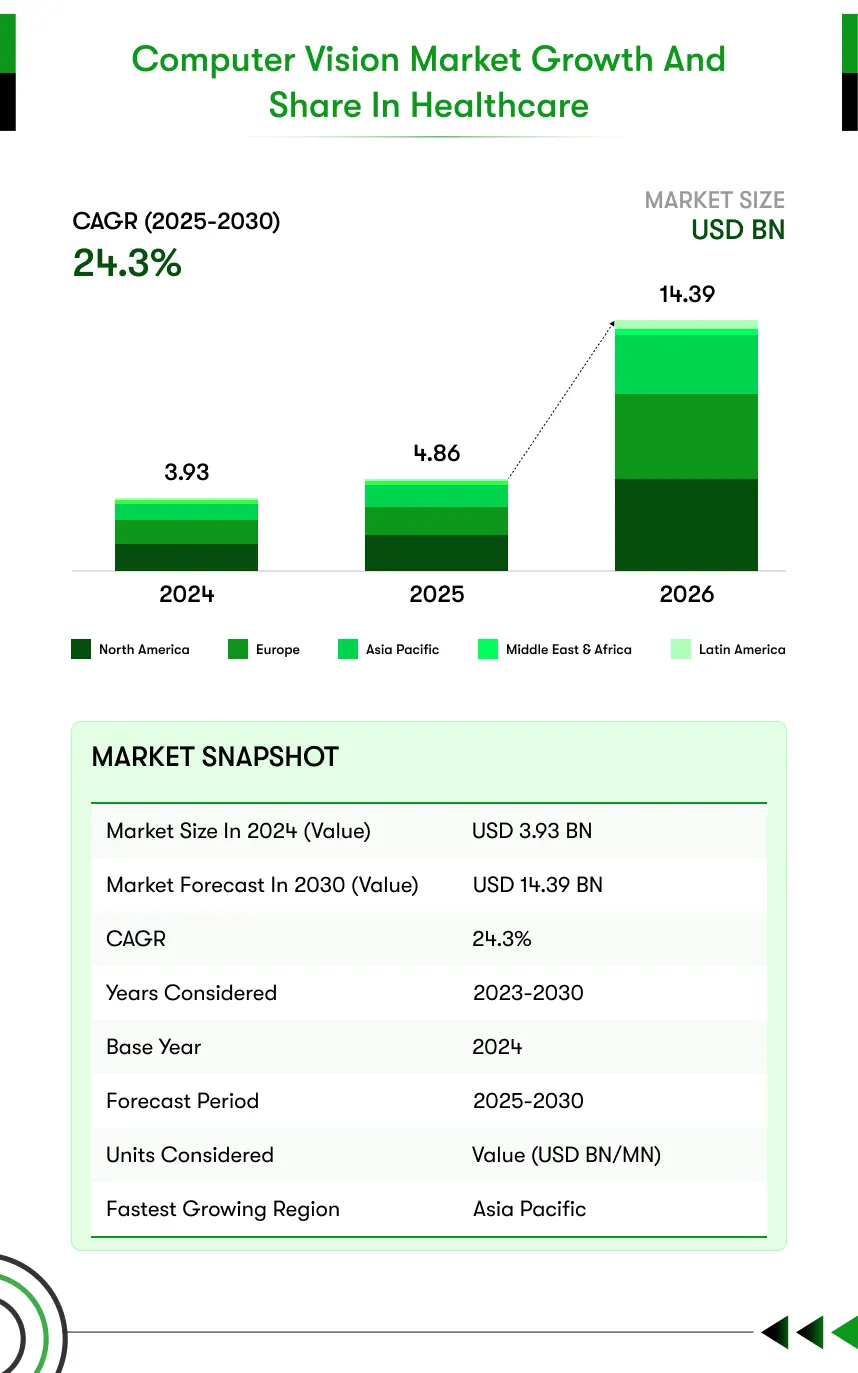
As case volume increases, more decisions stack up. More images enter the workflow, review time per case reduces, and small details become easier to miss under pressure. Healthcare systems are already moving toward structured image analysis to handle that demand, which is driving computer vision in the healthcare market from USD 4.86 billion in 2025 toward USD 14.39 billion by 2030.
Computer vision in healthcare brings consistency into that workload. Systems analyze medical images, highlight critical patterns, and help clinical teams manage higher volumes without missing key observations.
Across the computer vision in the healthcare industry, hospitals and diagnostic centers are applying AI-powered computer vision in healthcare where visual data directly impacts outcomes.
Ahead, you will see where computer vision in healthcare creates real operational impact and how you can apply it within your workflows.
Key Takeaways
- Computer vision significantly enhances diagnostic workflows by supporting consistent and accurate image interpretation across healthcare settings.
- AI-powered computer vision enables faster prioritization of critical cases and reduces the time required to analyze medical images.
- Organizations can scale visual data handling without increasing manual workload, improving operational efficiency across departments.
- Successful implementation requires thoughtful planning, high-quality data preparation, and alignment with healthcare infrastructure.
- Choosing a development partner with healthcare experience ensures smoother integration, regulatory compliance, and long-term support.
What is Computer Vision in Healthcare
Computer vision in healthcare refers to AI systems that analyze medical images and visual data to detect patterns, identify abnormalities, and support clinical decision-making across imaging, diagnostics, and monitoring workflows.
When you review a medical image, you rely on experience to interpret patterns and spot signals that indicate a condition. Computer vision brings that same pattern recognition into a system that processes images in a structured and consistent way.
These systems work on X-rays, CT scans, MRIs, pathology slides, and video feeds. Each image goes through the same level of analysis, which helps maintain consistency even when case volume increases.
Within computer vision use cases in the healthcare, these systems support your workflow by organizing visual data, highlighting key findings, and assisting in accurate interpretation across cases.
Why Healthcare Systems Are Struggling to Keep Up with Image Data and What Solves It
Healthcare needs computer vision to manage increasing volumes of medical images, reduce delays in diagnosis, improve consistency in interpretation, and support continuous monitoring where manual processes cannot scale effectively across high-demand clinical environments.
1. Increasing volume of medical images
Healthcare systems generate large volumes of imaging data across radiology, pathology, and screening workflows, which creates pressure on teams responsible for reviewing and interpreting these images.
- Diagnostic imaging demand continues to increase across hospitals and diagnostic centers.
- Screening programs generate repetitive image data that requires timely and accurate review.
- Multiple imaging modalities require parallel analysis, which increases workload across teams.
Growing image volume without proportional review capacity leads to delays and increased pressure across clinical workflows.
2. Limited availability of specialists
Image interpretation depends on trained professionals, but the number of specialists does not scale at the same rate as the growth in imaging demand.
- Radiology teams manage high case volumes, which reduces time available for each review.
- Pathology workflows require detailed manual analysis, which slows down processing speed.
- Screening programs often operate without consistent specialist coverage in many regions.
Limited specialist availability creates bottlenecks in workflows where accurate image interpretation is critical.
3. Delays in diagnosis and reporting
Time required to review medical images directly impacts how quickly healthcare providers can make clinical decisions and initiate treatment.
- Cases remain in queues before review, which delays diagnosis and decision-making.
- Urgent findings may not always receive immediate attention due to workload constraints.
- Reporting timelines extend across departments, which affects patient flow and care delivery.
Delays in image review extend the time between detection and treatment, which affects clinical outcomes, slows down care delivery, and increases pressure across healthcare systems.
4. Variability in manual interpretation
Manual image review introduces variation in outcomes based on experience, workload, and time constraints, which affects consistency in clinical decisions. This challenge highlights the role of computer vision in healthcare in bringing structured and repeatable analysis into image-driven workflows.
- Fatigue during extended shifts reduces consistency in image interpretation.
- Differences in clinical experience lead to variation in diagnostic conclusions.
- High-volume environments increase the risk of missing subtle details.
Variation in interpretation leads to inconsistent outcomes across cases, which affects diagnostic reliability, increases the need for re-evaluation, and reduces overall confidence in manual review processes.
5. Gaps in continuous monitoring
Healthcare environments require constant observation, which manual monitoring systems cannot sustain across large facilities and multiple departments.
- Patient safety monitoring depends on limited human observation capacity.
- Hygiene compliance tracking remains inconsistent without structured systems.
- Real-time monitoring becomes difficult to maintain at scale using manual processes.
Gaps in continuous monitoring reduce visibility into patient activity, safety risks, and operational compliance, which limits the ability to respond quickly to critical events.
Healthcare organizations require systems that can manage visual data at scale while maintaining accuracy and consistency across workflows. This requirement is driving adoption across computer vision in the healthcare industry.

How Computer Vision is Used in Healthcare and Where It Creates Real Clinical Impact
Computer vision in healthcare is applied across clinical and operational environments where image interpretation directly affects diagnosis, monitoring, and decision-making. Healthcare organizations use AI-driven systems to handle large volumes of visual data and bring structure into workflows that depend on consistent image analysis.
1. Radiology shows how computer vision is used in healthcare at scale
Radiology remains one of the most established areas for adoption, where systems assist in analyzing imaging data and supporting clinical decisions across high-volume environments.
- Systems detect abnormalities in X-rays, CT scans, and MRI images with consistent analysis.
- AI-powered computer vision in healthcare prioritizes cases where critical findings require immediate attention.
- Image segmentation isolates regions of interest for more focused clinical review.
This use case clearly demonstrates how computer vision is used in healthcare to manage high imaging volumes while improving consistency in interpretation.
2. Pathology highlights the role of computer vision in healthcare for detailed analysis
That workflows rely on microscopic image evaluation, where structured analysis improves how tissue samples are reviewed across cases.
- Systems identify regions of interest within digital pathology slides for detailed examination.
- Image classification supports detection of abnormal cell structures across samples.
- Quantitative analysis measures tissue characteristics for consistent evaluation.
Pathology workflows handle large volumes of slides where each sample requires detailed review. Structured image analysis helps maintain uniform evaluation across cases and reduces the time required to identify regions that need closer examination.
3. Ophthalmology shows the benefits of computer vision in healthcare for screening
Retinal imaging workflows support large-scale screening programs where early detection plays a critical role in patient outcomes.
- Systems analyze retinal images to detect indicators of diabetic retinopathy and related conditions.
- Screening programs use automated image analysis to expand coverage beyond specialist-dependent environments.
- Consistent evaluation across large populations supports structured screening programs.
Ophthalmology workflows show how screening programs can expand while maintaining reliable analysis.
4. Dermatology expands image-based diagnosis into remote care
Skin image analysis represents a growing segment in the market, especially in remote care and telemedicine environments.
- Systems evaluate skin lesions and identify visual patterns associated with different conditions.
- Image comparison tracks progression of skin conditions over time.
- Remote analysis supports virtual consultations and distributed care models.
Dermatology applications indicate how the computer vision in the healthcare market continues to expand across diagnostic and remote care workflows.
5. Surgical workflows support real-time decision-making
Procedural environments require immediate visual interpretation, where systems assist clinicians during live workflows.
- Systems detect anomalies during procedures such as colonoscopy and endoscopy.
- Real-time image analysis supports decision-making during critical stages of procedures.
- Visual overlays assist clinicians in understanding anatomical structures during operations.
Surgical workflows reflect how computer vision is used in healthcare to support precision and awareness during time-sensitive procedures.
6. Hospital operations improve monitoring and safety
Procedural environments require immediate visual interpretation, where systems assist clinicians during live workflows.
- Systems monitor patient movement to detect fall risks and unusual activity patterns.
- Video analysis supports hygiene compliance tracking across departments.
- Real-time monitoring improves visibility across large hospital environments.
Operational use cases demonstrate how computer vision in healthcare supports safety, monitoring, and workflow visibility beyond diagnostic environments.
Image-heavy workflows across healthcare are not slowing down. Radiology, pathology, screening programs, and hospital operations continue to depend on accurate visual interpretation at scale. Computer vision for airports & transport hubs fits into these environments as a structured layer that supports faster review, clearer prioritization, and consistent decision-making across growing case volumes.

What Benefits Does Computer Vision in Healthcare Deliver Across Clinical Workflows
Healthcare systems are overwhelmed with an increasing volume of medical images, leading to delayed diagnoses, inconsistent results, and overburdened professionals. Computer vision in healthcare offers a way out by helping teams analyze visual data with greater speed, consistency, and accuracy.
1. Faster identification of critical findings
The ability to identify critical findings early can make all the difference in patient outcomes, especially in time-sensitive conditions. With AI-powered computer vision in healthcare, systems can automatically prioritize images for urgent review, enabling clinicians to make faster decisions and improving response time in critical situations.
Faster identification supports decision-making in emergency radiology workflows, stroke assessment pathways, and cancer screening programs where time directly affects outcomes.
Where impact is visible:
- Radiology workflows prioritize CT and MRI scans that contain critical findings such as hemorrhage or stroke indicators.
- Emergency department workflows reduce waiting time for imaging review during acute care situations.
- Oncology screening workflows accelerate detection of suspicious patterns that require further evaluation.
2. Improved consistency in image interpretation
Manual interpretation varies based on workload, experience, and time constraints. Computer vision in healthcare applies the same analytical process across every image, which improves consistency in interpretation.
AI-powered computer vision in healthcare supports standardized analysis across radiology, pathology, and screening workflows where variation can affect diagnostic accuracy.
Where consistency improves:
- Radiology reporting workflows maintain uniform interpretation across different clinicians and shifts.
- Pathology workflows reduce variation in slide analysis across multiple reviewers.
- Population screening workflows ensure consistent evaluation across large patient datasets.
3. Higher patient throughput without increasing workload
Healthcare systems face increasing case volumes without proportional increases in specialist availability. Computer vision in healthcare helps teams handle more cases by reducing time spent on repetitive analysis.
Improved throughput supports radiology departments, diagnostic centers, and screening programs that operate under continuous demand.
Where throughput improves:
- Radiology departments process higher volumes of imaging studies without extending reporting timelines.
- Diagnostic imaging centers reduce turnaround time per scan while maintaining quality.
- Screening programs manage large datasets without increasing dependency on specialist review capacity.
4. Expanded reach of screening programs
Screening programs often depend on specialist availability, which limits coverage in many regions. Computer vision in healthcare supports image-based screening that can operate across different care settings.
The benefits of computer vision in healthcare become visible in large-scale screening programs that require consistent evaluation across distributed locations.
Where screening expands:
- Primary care screening workflows operate in locations without on-site specialists.
- Community health programs extend screening services into rural and underserved regions.
- Mobile screening units use automated analysis to maintain consistent evaluation across populations.
5. Reduced manual workload across clinical teams
Clinical teams are often overwhelmed by repetitive, time-consuming tasks, leading to burnout and reduced efficiency. Automating routine image analysis that reduces manual effort, freeing up specialists to focus on higher-level tasks and improving overall workflow efficiency.
Where workload reduces:
- Radiology workflows automate initial image analysis to reduce repetitive review tasks.
- Pathology workflows reduce manual effort in identifying regions of interest on slides.
- Screening workflows minimize repetitive evaluation steps across large patient datasets.
6. Improved monitoring and operational visibility
Healthcare facilities require continuous monitoring for patient safety and operational efficiency.
Structured visibility supports hospital safety teams, facility management, and compliance workflows that depend on real-time observation.
Where visibility improves:
- Patient safety workflows detect movement patterns that indicate fall risk in hospital wards.
- Infection control workflows monitor hygiene compliance across clinical environments.
- Facility operations workflows maintain real-time visibility across large hospital infrastructures.
Faster image review, consistent interpretation, and scalable screening define how computer vision improves healthcare workflows. Clinical teams handle higher volumes with better accuracy while maintaining decision quality across departments.
These advancements are key to building a robotic healthcare infrastructure that supports seamless operations. The next section explains the challenges that healthcare organizations must address before implementing computer vision at scale.

What Challenges Should You Expect When Implementing Computer Vision in Healthcare
Implementing computer vision in healthcare involves more than model development. Healthcare environments require accuracy, compliance, integration, and reliability across real workflows. Each stage of implementation introduces challenges that organizations must address before scaling solutions across clinical and operational systems.
1. Data quality and availability directly affect performance
Computer vision systems depend on high-quality medical images and well-structured datasets. Inconsistent, incomplete, or poorly labeled data reduces model reliability and limits clinical usefulness.
Where challenges appear:
- Medical imaging datasets often vary across devices, formats, and institutions.
- Annotation requires clinical expertise, which increases time and cost.
- Limited access to diverse datasets affects performance across different patient groups.
Data limitations create gaps in performance when systems move from controlled environments to real clinical settings.
2. Clinical Validation
Clinical validation of computer vision systems is a time-consuming and rigorous process. Systems must demonstrate their ability to deliver reliable, accurate results before they can be adopted for widespread clinical use.
- Testing models across multiple datasets and real-world scenarios is essential for validation.
- Performance in clinical environments may differ from controlled settings, requiring further refinements.
- Clear evidence of improved clinical outcomes is needed to gain healthcare providers’ trust.
Clinical validation ensures that computer vision technology can be safely integrated into medical workflows, directly impacting patient care and treatment decisions.
3. Integration with Existing Systems
Integrating new technologies into existing healthcare infrastructures can be a significant hurdle. Healthcare environments often rely on multiple systems (like PACS, EHRs, and imaging software) that must be compatible with AI-powered computer vision tools.
- Systems must work seamlessly with legacy platforms and clinical workflows.
- Data exchange standards vary across institutions, making integration complex.
- Collaborative efforts between clinical and technical teams are crucial for smooth implementation.
Integration is critical for ensuring that the technology is not just adopted but enhances existing processes without disrupting clinical operations.
4. Regulatory and Compliance Challenges
Meeting regulatory standards is one of the major obstacles to deploying computer vision systems in healthcare. Since healthcare data is highly sensitive, there are strict requirements governing how it is accessed, used, and shared.
- Systems must meet FDA approval and comply with other regional regulations.
- Data privacy regulations like HIPAA in the U.S. require robust security measures to protect patient information.
- Detailed documentation and audit trails are needed for compliance verification.
Regulatory approval ensures that computer vision solutions are not only effective but also safe for clinical use.
5. Trust and Adoption Among Clinicians
For any new technology to succeed, clinical staff must trust it. Since many healthcare providers are used to traditional methods of image analysis, introducing AI-based solutions can meet resistance if the benefits aren’t clear.
- Clinicians require transparency in how AI models make decisions.
- Resistance to new technology is common in healthcare, and overcoming it requires clear proof of benefit.
- Proper training and clear communication are essential for smooth adoption.
Building trust and ensuring that computer vision systems align with clinicians’ workflows are vital for successful adoption.
6. Scalability and Real-World Performance
Healthcare systems vary in terms of infrastructure, resources, and patient demographics. As computer vision technology expands, systems must be scalable to handle increasing volumes of data and different types of imaging.
- Performance can vary depending on imaging standards and equipment across institutions.
- Infrastructure must be capable of processing large amounts of data efficiently.
- Continuous system monitoring is required to ensure that performance remains reliable at scale.
Scalability ensures that the technology can grow alongside healthcare systems and continue providing value as demand increases.
The challenges of implementing computer vision in healthcare may seem daunting, but with proper planning and resources, they can be overcome. Addressing these challenges allows healthcare organizations to unlock the full potential of computer vision technology, such as how computer vision is used in Medigo, to improve patient care, workflow efficiency, and diagnostic accuracy.
What You Need to Know Before Implementing Computer Vision in Healthcare
Implementing computer vision in healthcare requires a structured, step-by-step approach to integrate it effectively into clinical workflows. The technology promises to improve diagnostic accuracy, speed, and efficiency, but its adoption requires clear planning, collaboration across teams, and the right technology stack.

1. Define Clear Use Cases and Objectives
Before implementing computer vision, it’s essential to define the use cases where the technology will have the most impact. From radiology to pathology, identifying key workflows will allow healthcare organizations to focus their efforts where the technology can offer the greatest value.
- Identify high-priority areas like radiology, dermatology, or screening programs.
- Align use cases with operational goals (e.g., reducing diagnostic time, increasing throughput).
- Ensure the technology will complement existing clinical workflows, not disrupt them.
By aligning computer vision with specific needs, organizations can ensure it delivers measurable benefits.
2. Ensure Data Quality and Availability
Data is the foundation of AI-powered computer vision. To train models accurately, healthcare organizations need high-quality, standardized datasets. Poor data quality will lead to inaccurate results and reduce the system’s effectiveness in clinical environments.
- Collect medical images across multiple modalities (X-rays, CT scans, MRIs) to build a diverse dataset.
- Ensure data annotation is done accurately by clinical experts to ensure reliable training models.
- Address privacy and compliance concerns when using patient data for training purposes (e.g., HIPAA compliance).
High-quality data is necessary for building robust AI models that perform consistently across different clinical settings.
3. Choose the Right Computer Vision Technology
Selecting the right computer vision technology is crucial for successful implementation. Different systems offer varying capabilities, and choosing the wrong solution can lead to inefficiencies or poor integration.
- Choose an AI-powered computer vision platform that integrates easily with your existing healthcare infrastructure (e.g., PACS, EHR).
- Look for solutions that provide scalability, allowing the system to expand as the healthcare facility grows.
- Ensure the technology can handle the specific clinical needs of your organization, whether for diagnostics or monitoring.
Selecting the right technology enables seamless integration and helps maximize the return on investment (ROI).
4. Validate and Test the System
After selecting the technology, clinical validation is essential before full deployment. Testing the system in real-world environments ensures that it performs as expected and meets the regulatory standards required in healthcare.
- Conduct pilot projects in controlled environments to assess system performance and accuracy.
- Validate the AI models using clinical data from actual patient cases.
- Continuously assess the technology’s ability to improve outcomes and reduce time-to-diagnosis.
Clinical validation ensures the technology meets the highest standards of healthcare delivery and patient safety.
5. Train and Onboard Clinical Teams
Successful implementation of computer vision requires buy-in from clinical staff. It’s critical to ensure that healthcare providers understand how the system works, including how the health screening robot fits into their daily workflow and enhances patient care.
- Provide training to clinicians, ensuring they understand how the system enhances their decision-making process.
- Demonstrate the value of the technology with real-world examples and success stories.
- Address concerns by showing how the technology supports existing practices rather than replacing clinicians.
Effective training drives adoption and helps integrate computer vision into clinical workflows smoothly.
6. Monitor and Optimize the System Continuously
Implementing computer vision doesn’t stop after deployment. Continuous monitoring is required to ensure the system stays accurate, reliable, and aligned with clinical goals.
- Set up a monitoring system to track performance across departments and imaging modalities.
- Ensure continuous model updates to keep up with new data and advancements in medical imaging.
- Gather feedback from clinicians to identify areas for improvement and further optimization.
Regular monitoring and updates help maintain system performance and ensure its long-term success.
Implementing computer vision in healthcare requires overcoming various challenges, such as ensuring data quality, meeting regulatory compliance, and achieving smooth integration with existing systems.
When healthcare organizations follow these steps, they unlock the full potential of computer vision in healthcare, leading to faster, more accurate diagnostic workflows and enhanced patient care.
How to Choose the Right Computer Vision Development Partner
Choosing the right computer vision development partner is a critical step in successfully implementing AI technology in healthcare. The right partner will have the expertise, tools, and understanding to meet your specific needs, integrate seamlessly with existing systems, and drive long-term success.
1. Look for Expertise in Healthcare Applications of Computer Vision
The ideal development partner should have significant experience in applying computer vision to healthcare-related tasks, such as medical imaging, diagnostics, and patient monitoring.
Why this matters:
- A partner with experience in AI-powered computer vision in healthcare can better understand the nuances of healthcare workflows.
- They can help identify and customize solutions that address specific healthcare challenges, ensuring smoother integration and quicker deployment.
- Clinical expertise in the team ensures the system is built around healthcare needs and regulatory requirements.
2. Assess Technical Competency and Innovation
Not all computer vision systems are built the same. Evaluate the technical capabilities of potential partners, including the robustness of their AI models and their ability to scale the technology as your organization grows.
Why this matters:
- A partner with cutting-edge technology ensures the system is both scalable and adaptable.
- Innovation is key in a fast-evolving field like computer vision, and your partner should have a forward-thinking approach to AI-powered solutions in healthcare.
- Assess their ability to work with the latest machine learning algorithms and handle large volumes of healthcare data.
3. Ensure Strong Integration Capabilities
Integrating new technology into existing healthcare infrastructure is a complex task. The right partner should have a proven track record of working with systems like PACS, EHR, and other clinical data management tools.
Why this matters:
- Seamless integration with existing workflows is essential to avoid disruption and maximize operational efficiency.
- Data interoperability ensures that your computer vision system communicates smoothly with other healthcare systems and platforms.
- Effective integration helps avoid costly delays and errors during deployment.
4. Verify Experience with Regulatory Compliance
Healthcare technologies must comply with strict regulatory standards such as HIPAA and FDA approval for medical devices. A reliable development partner should be familiar with these regulations and ensure the system complies.
Why this matters:
- Regulatory compliance is non-negotiable in healthcare. A partner with experience in regulatory compliance ensures your system meets necessary legal and privacy standards.
- They will guide you through the certification process, helping you avoid costly mistakes and delays.
5. Consider the Partner’s Support and Maintenance Offerings
After implementation, continuous support and maintenance are essential to ensure the system operates smoothly. The right partner will offer ongoing technical support, model updates, and system optimizations.
Why this matters:
- Post-deployment support is crucial for addressing issues that arise after the system is live.
- Regular updates and maintenance ensure that the system stays up to date with the latest medical advancements and continues to meet healthcare needs.
- Training for healthcare professionals ensures the system is used effectively in daily clinical workflows.
6. Review Pricing and Contract Terms
Pricing is always an important consideration when choosing a development partner. It’s essential to ensure that the pricing structure fits within your budget while not sacrificing quality or support.
Why this matters:
- Cost transparency is key to avoiding hidden fees and ensuring that you understand what is included in the contract.
- You need a partner that offers flexible pricing models that fit your organization’s scale and needs, whether for initial deployment or ongoing support.
7. Check References and Case Studies
Finally, reviewing a potential partner’s references, case studies, and past work in healthcare will give you a better sense of their capabilities and the impact they’ve had on previous projects.
Why this matters:
- A partner’s past success in healthcare computer vision projects shows their ability to deliver on promises.
- Client feedback and case studies give you a real sense of the partner’s approach, reliability, and the results they can help you achieve.
Look for a partner with experience in both AI-powered computer vision and healthcare-specific applications. Focus on technical expertise, smooth integration, regulatory knowledge, and long-term support to ensure that the technology enhances your organization’s workflow and ultimately improves patient outcomes.

Conclusion
As healthcare organizations face increasing pressure to enhance diagnostic accuracy, improve efficiency, and provide better patient care, computer vision in healthcare is quickly becoming a game-changer. This blog has outlined how AI-powered computer vision can streamline workflows, reduce manual workload, and increase diagnostic precision across various healthcare applications, from radiology to surgery.
Choosing the right computer vision development partner is critical in ensuring successful implementation, and we’ve provided a roadmap to help you navigate that decision. Whether it’s gathering high-quality data, ensuring compliance, or integrating seamlessly with existing systems, the right partner will be your key to unlocking the full potential of this transformative technology.
At Kody Technolab, we specialize in custom-built computer vision solutions designed specifically for the healthcare industry. Our team of experts will guide you through the entire process—from strategy and development to deployment and support. If you’re ready to innovate and elevate your healthcare operations, contact us today to discuss how we can help you achieve your goals with cutting-edge computer vision technology.
FAQs About Computer Vision in Healthcare
1. What is computer vision in healthcare and how does it work?
Computer vision in healthcare uses AI to analyze medical images like X-rays, CT scans, and MRIs. It detects patterns and abnormalities to help clinicians make more accurate and timely diagnoses. The technology works by processing large datasets of images to recognize important features that aid decision-making.
2. How can computer vision improve patient care in healthcare?
Computer vision improves patient care by speeding up the analysis of medical images, ensuring faster diagnoses. It reduces errors, improves the accuracy of findings, and helps detect conditions earlier, ultimately leading to better patient outcomes.
3. What are the benefits of implementing AI-powered computer vision in healthcare?
Implementing AI-powered computer vision enhances diagnostic speed, boosts accuracy, and increases operational efficiency. It helps healthcare systems scale to handle more patients without sacrificing quality, all while improving patient safety through faster detection of conditions.
4. How do I integrate computer vision systems into existing healthcare workflows?
To integrate computer vision, select systems that fit seamlessly with existing healthcare infrastructure like PACS or EHRs. Ensure the technology aligns with clinical workflows and provide training to staff on how to use the system effectively alongside their regular tasks.
5. What challenges do healthcare organizations face when implementing computer vision?
Healthcare organizations face challenges like ensuring high-quality, well-annotated data, integrating new systems with existing infrastructure, ensuring regulatory compliance, and getting clinician buy-in for new technology. These challenges must be addressed to maximize the effectiveness of computer vision.
6. Is computer vision in healthcare compliant with medical regulations like HIPAA?
Yes, computer vision systems used in healthcare must adhere to HIPAA and other data privacy regulations to ensure that patient data is handled securely and in compliance with healthcare laws.
7. What is the future of computer vision in healthcare?
The future of computer vision in healthcare lies in even more advanced AI models capable of real-time surgical assistance, enhanced diagnostic accuracy, and greater use in preventive care. These innovations will improve both the quality and speed of patient care.
8. How much does it cost to implement computer vision in healthcare?
Costs vary depending on the scope of the implementation, but the return on investment (ROI) is significant. The technology can reduce diagnostic delays, increase efficiency, and lower long-term operational costs, making it a worthwhile investment.
9. Can computer vision be used in remote healthcare settings?
Yes, computer vision can be applied in telemedicine and mobile health applications, enabling remote diagnostics, especially in underserved areas. It ensures that more people have access to timely medical assessments and care, even without specialist availability.
10. How can my organization get started with computer vision in healthcare?
Start by identifying specific use cases in your organization where computer vision can be applied (e.g., radiology or pathology). Partner with a reliable development team, gather high-quality data, run pilot tests, and ensure that clinical staff is trained on how to use the system.












 Contact Information
Contact Information