Key takeaways
- Preventive healthcare infrastructure is becoming a high-growth, data-driven priority for long-term cost efficiency and resilience.
- Traditional, facility-based screening models cannot scale across distributed workforces and underserved populations.
- Early detection reduces treatment costs, improves productivity, and strengthens organizational risk management.
- The future model is AI-powered, always-on, and accessible across everyday, high-footfall environments.
- Robotic and automated screening enables scalable deployment without increasing manpower or infrastructure costs.
- Digital systems turn screenings into real-time, centralized health intelligence for better decision-making.
- AI diagnostics, telemedicine, and personalized insights enable faster intervention and more effective outcomes.
- Future-ready infrastructure combines distributed access, predictive intelligence, and scalable, sustainable models.
The future of Preventive Healthcare Infrastructure is changing rapidly. The worldwide market is projected to hit USD 585.6 billion by the year 2030 at an astounding rate of 11.8% per year. However, the systems that many organizations continue to use, which are fixed clinics, appointments, and staff-intensive screening, are not the systems of the current time.
Today, they are unable to support remote workers and rural groups, as well as a world that requires constant tracking of their health. Consequently, millions of people do not receive early diagnosis of diseases that can be prevented, such as diabetes and heart disease.
This growing gap is pushing leaders across industries to rethink their approach. The focus is shifting toward smarter, more flexible solutions like AI-powered and robotic systems that can deliver diagnostics anytime, anywhere.
These innovations not only enhance access but also save money, provide real-time information, and help lead to healthier communities. It is not only futuristic to invest in modern Preventive Healthcare Infrastructure, but it is also increasingly becoming the key to long-term effects and resilience.
What is Preventive Healthcare and Why Does It Matter for Organizations?
Preventive healthcare is the practice of identifying and addressing health risks before they become serious, costly, or life-threatening conditions. It is the systematic chnage from treating illness after it occurs to detecting and intervening before it progresses.
For individuals, preventive healthcare means catching conditions like diabetes, hypertension, and cardiovascular disease at a stage when they are manageable, reversible, and inexpensive to treat. For organizations and governments, it means a workforce that is healthier, more productive, and less likely to generate catastrophic medical costs downstream.
The World Bank estimates that every USD 1 invested in preventive health interventions yields USD 4 to 9 in long-term treatment cost savings. Companies that implement structured preventive wellness programs reduce absenteeism by up to 30% and healthcare costs by up to 25% within two years, according to occupational health research. The financial case for prevention is not marginal. It compounds with every year of early detection.
Despite this, the global system remains structurally skewed toward reactive treatment. The WHO estimates that 60% of deaths in low and middle-income countries are attributable to conditions that early screening could have identified and addressed. The infrastructure gap is not a knowledge problem. It is a delivery problem, and closing it requires a fundamentally different approach to how and where screening happens.
What Does the Future of Preventive Healthcare Infrastructure Actually Look Like?
The future of preventive healthcare infrastructure is deployable, data-driven, AI-powered, and continuous. It is not built around fixed facilities, scheduled appointments, or dedicated staff. It is built around one simple principle: screening should reach people wherever they are, not wherever a clinic happens to exist.
Three structural shifts are already redefining what modern preventive health infrastructure looks like on the ground:
- From facilities to footfall: High-traffic locations like corporate campuses, transit hubs, pharmacies, community centers, and rural health points are no longer passive waiting spaces. They are becoming an active screening infrastructure that meets people in the flow of their everyday lives.
- From fragmented records to unified intelligence: Every screening feeds a centralized, real-time dashboard that organizations and governments can act on immediately, replacing disconnected silos with a single, live view of population health.
- From appointment-dependent to always-on: The future of preventive healthcare is not something people schedule around their symptoms. It is something they interact with regularly, consistently, and without friction, long before a condition demands urgent attention.
This is not a distant vision waiting to be built. The digital preventive healthcare systems, AI diagnostics, and autonomous screening infrastructure that make this possible already exist and are already operational. The organizations and governments that act on this now will build a measurable and compounding advantage in workforce health, public health outcomes, and long-term cost efficiency.
Robotic Healthcare Infrastructure: The Deployable Backbone.
One of the more important facilitators of this future is the robotic healthcare infrastructure, with autonomous screening robots transforming ordinary spaces into 24/7 health stations. These AI-powered robots, systems, and sophisticated kiosks with biometric measurements, blood tests, and scanning are installed in public health centers, factories, offices, shopping centers, or distant clinics within days. The deployment is a crucial pillar, and organizations adapting to the futuristic preventive healthcare infrastructure are positioning themselves ahead of the rest of the industry.
Examples in the real world are the Henn-na Hotel robots in Japan to check the health of guests and the trial of robotic kiosks in Singapore to check the health of 1,000+ residents weekly (95% accuracy on hypertension and diabetes). Manufacturing companies, such as Foxconn, also incorporate them into production lines, where they are exposed to fatigue-related hazards before the shift. This is an exponentially scaling robotic layer: a single unit would be the output of a clinic at 1/10 the cost, with the output fed to dashboards to predict the health of the workforce.
In the case of organizations, it is a force multiplier that spreads preventive care to 100 percent of locations without a linear rise in costs.
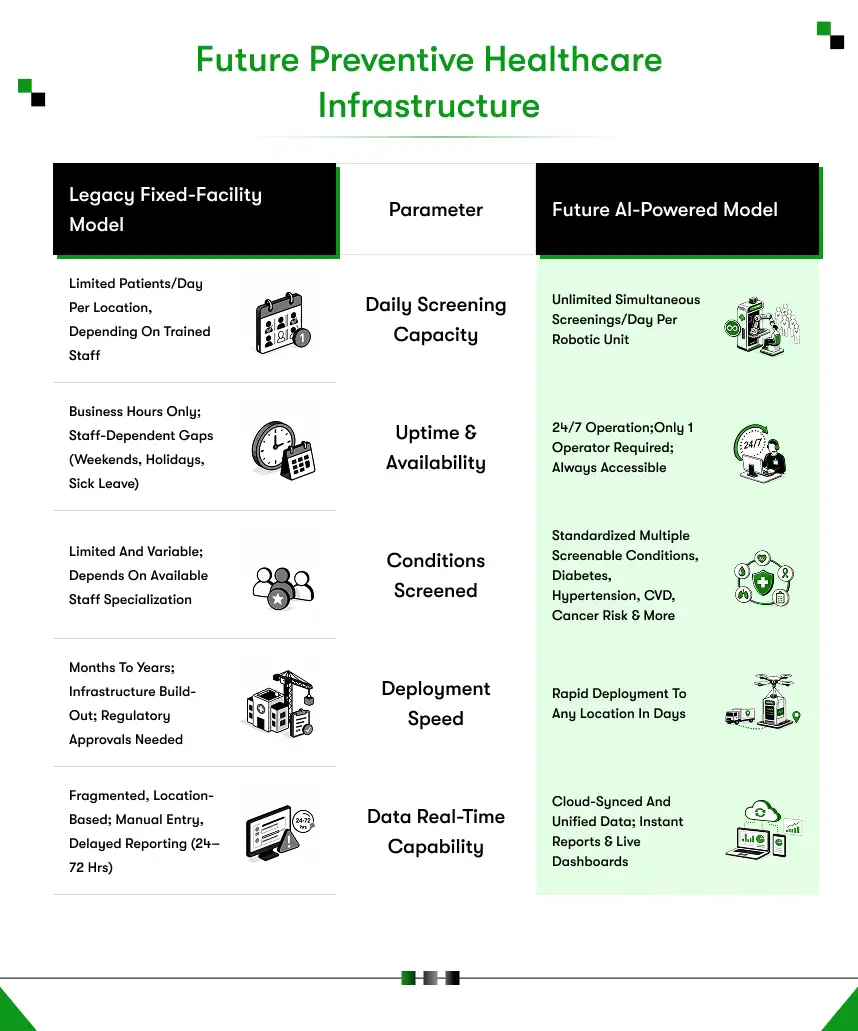
Why Is the Current Preventive Health Infrastructure Model Failing at Scale?
The current preventive health infrastructure model fails at scale because it was designed for a different era. It assumes that people will travel to facilities, book appointments in advance, and access screening through a trained professional. Every one of those assumptions breaks down when you try to scale across multiple locations, geographies, or large populations.
| Failure Point | What It Looks Like Today | The Cost of Inaction |
| Geographic Limitation | Screening only exists where physical facilities are located. | Billions of people never access life-saving early detection. |
| Data Fragmentation | Health records are siloed by specific location and provider. | No unified picture of population or workforce health trends. |
| Human Dependency | Screening services stop when staff are unavailable or off-shift. | Inconsistent access, scheduling gaps, and high operational costs. |
| Appointment Friction | It takes days or weeks to secure a screening slot. | Preventive care is deferred until symptoms become acute. |
| Scaling Cost | Each new location replicates the full infrastructure cost. | Organizations cannot afford to scale services equitably. |
The numbers tell the story clearly. In rural India, the doctor-to-patient ratio exceeds 1 to 10,000. Average lab report turnaround in developing economies runs 24 to 72 hours. The average diagnostic spend per screening episode ranges from USD 30 to USD 120. These are not outliers. They are the structural reality of a system that was never designed to scale.
For enterprise decision makers, the failure is equally visible. A large organization running a health lounge at its headquarters screens less than 15% of its total workforce annually, because four out of five employees work at sites with no screening infrastructure at all. The health data that leadership needs to make informed workforce decisions simply does not exist because the model cannot reach far enough to generate it.
How Is Digital Preventive Healthcare Reshaping the Way Organizations Screen at Scale?
Digital preventive healthcare systems are reshaping screening by removing the three dependencies that have always limited scale: physical space, human operators, and appointment-based access. When those dependencies are removed, screening can happen anywhere, at any time, for any number of people simultaneously.
According to Deloitte’s 2026 US Health Care Outlook, nearly 60% of health plan and health system executives intend to invest in virtual health services to improve preventive care. More than 50% of health plan executives plan to expand digital tools for member engagement and health monitoring. These are not aspirational numbers. They reflect a capital allocation decision that has already been made at the executive level across the industry.
At the operational level, digital preventive healthcare systems change how screening data is generated, stored, and used. Instead of paper-based or siloed electronic records that live inside a single facility, digital systems generate standardized, real-time data that feeds directly into organizational and population health dashboards. Leadership moves from making workforce health decisions based on incomplete annual reports to making them based on live intelligence updated with every screening session.
For governments, the upgrade is even more significant. Real-time population health data enables predictive resource allocation, early epidemic detection, and evidence-based policy decisions at a scale and speed that no legacy infrastructure can match. The move to digital preventive healthcare infrastructure is not a technology upgrade. It is a governance capability upgrade.
What Role Does Automated Health Screening Infrastructure Play in the Future of Prevention?
Automated health screening infrastructure is the operational backbone of modern preventive care. It is what makes the future of preventive healthcare infrastructure physically real, not just conceptually compelling. Without automation, the vision of always-on, everywhere-accessible screening remains theoretical.
A health screening robot removes every operational constraint that limits a traditional screening model. It requires no trained operator on duty. It does not depend on appointment availability. A health screening robot does not need a dedicated room or fixed location. It operates in any high-footfall environment and delivers a comprehensive health report in minutes, not days.
The role of Robotics in Healthcare in this context is not to replace clinicians. It is to extend the reach of early detection to every location and every population that a clinician cannot physically serve at scale. A hospital cannot be everywhere. A deployable screening robot can.
The scale implications are significant. One automated health screening unit creates the screening capacity of a full primary care clinic, without the overhead, without the staffing dependency, and without the geographic constraint. For an organization managing 10 sites, a fleet of 10 units delivers uniform screening access across the entire workforce simultaneously, feeding all results into a single centralized dashboard.
For governments deploying automated health screening infrastructure at the community level, the impact compounds differently. Every unit deployed adds to a real-time national health intelligence layer, building a living picture of population health that drives faster, smarter public health decisions.

How Does Robotic Preventive Healthcare Infrastructure Change the Economics of Early Detection?
Robotic preventive healthcare infrastructure does not just make early detection cheaper. It fundamentally changes what early detection can do for an organization and what it costs when it is absent. The financial case stops being about line items the moment you look at what happens on the ground.
Consider what the practical difference looks like:
Reach replaces scarcity:
A traditional preventive health infrastructure model serves the employees who are physically close to it. Robotic healthcare kiosks deployed across every site serve the entire workforce, not just the 10 or 15 percent who happen to be near a health lounge. When you close that gap, you stop missing the conditions that go undetected simply because someone never had a reason to walk into a clinic.
Consistency replaces variability:
A health screening robot does not have off days, staffing shortages, or appointment backlogs. Every employee who steps up to a unit gets the same quality of screening, the same comprehensive output, and the same instant access to results, whether they are at the headquarters or a remote facility.
Prevention replaces crisis management:
The real economic shift that robotic healthcare infrastructure drives is upstream. When a condition like hypertension, diabetes risk, or early cardiovascular strain is caught at a routine screening rather than an emergency admission, the organization is not managing a crisis. It is avoiding one entirely, which changes the cost conversation at every level.
Intelligence replaces assumption:
When you compare a Health Lounge vs Health Screening Robot model, the difference is not just cost per session. It is the quality of organizational intelligence generated. Robotics in Healthcare at this scale turns screening into a continuous data asset, enabling proactive wellness investment instead of reactive claims management.
Scale replaces ceilings:
The legacy model hits a cost ceiling the moment you try to expand it. Robotic preventive healthcare infrastructure does not. A single additional unit adds a full new screening capability without replicating the staffing, space, or operational overhead that made the old model unaffordable to scale.
The change from automated health screening infrastructure to strategic health intelligence is not theoretical. It is the practical outcome of deploying a model that was built to reach everyone, not just the people already close to care.
What Are the Key Pillars of a Future-Ready Preventive Healthcare Infrastructure?
A future-ready preventive healthcare infrastructure is built on seven pillars. Each one addresses a specific failure of the legacy model, and together they define what scalable, intelligent, and equitable preventive care looks like in practice.
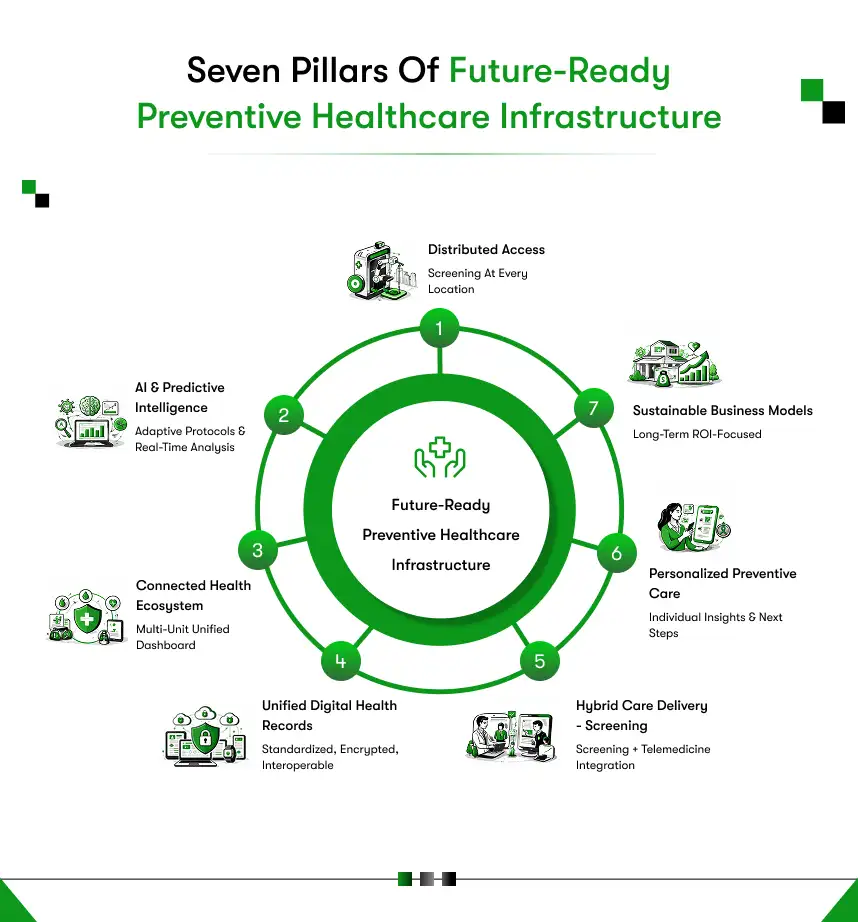
| Pillar | What It Means in Practice | Medigo Delivers This |
| Distributed Access Infrastructure | Screening units are deployed to offices, kiosks, pharmacies, transit hubs, and rural centers. | Yes, fully deployable to any high-footfall location. |
| AI and Predictive Intelligence | AI interprets results, adapts protocols, and flags anomalies in real time. | Yes, proprietary adaptive protocol engine and clinical AI layer. |
| Connected Health Ecosystem | Multi-unit deployments share data on one organizational dashboard, fully siloed. | Yes, a centralized, encrypted dashboard per organization. |
| Unified Digital Health Records | Standardized data with built-in privacy and data sovereignty architecture. | Yes, cloud-synced, encrypted, government and enterprise-grade. |
| Hybrid Care Delivery | Telemedicine is integrated into the same screening session as physical diagnostics. | Yes, real-time physician consultation and digital prescription are built in. |
| Personalized Preventive Care | Post-screening analysis delivers individual insights and recommended next steps. | Yes, post-result analysis with plain-language personalized guidance. |
| Sustainable Business Models | Organizations purchase infrastructure that delivers long-term preventive care ROI. | Yes, the direct buy model positioned as a long-term infrastructure asset. |
1. Distributed Access Infrastructure
The first pillar is physical reach. Preventive healthcare infrastructure must exist where people already are, not where they are expected to travel. Robotic healthcare kiosks deployed across corporate campuses, pharmacies, transit nodes, and rural health centers transform passive spaces into active screening points. The infrastructure follows the population, and every new deployment point expands the reach of early detection without replicating fixed facility costs.
2. AI and Predictive Intelligence
The second pillar is intelligence. AI does not just interpret screening results. It adapts the screening protocol based on individual responses and demographics, flags anomalies in real time, and builds a predictive layer that identifies health risks before they become conditions. This adaptive intelligence is what separates a genuinely scalable screening system from a digitized version of a manual process.
3. Connected Health Ecosystem
The third pillar is connectivity within organizational boundaries. When multiple screening units are deployed across different locations within the same organization, every result feeds into a single, centralized dashboard. Leadership sees a unified health picture across the entire organization in real time. Critically, this connectivity is fully siloed. One organization’s health data is completely inaccessible to any other organization. Each institution owns and controls its own health intelligence exclusively, with no cross-organizational data exposure under any circumstance.
4. Unified Digital Health Records
The fourth pillar is data integrity and privacy. Screening data must be standardized, encrypted, and built for interoperability with existing health record systems. Data sovereignty must be guaranteed at the government and institutional level. Every screening result that enters the system must be protected with the same rigor as any sensitive medical record, and the architecture must be designed so that privacy is structural, not a policy afterthought.
5. Hybrid Care Delivery
The fifth pillar is the integration of physical screening with immediate clinical access. A comprehensive screening session is only as useful as the action it enables. When a screening result flags a critical value, the individual must be able to connect with a physician instantly, within the same session, without being redirected to a separate booking system or a different facility. Telemedicine integrated directly into the screening process is what turns a data point into a care pathway.
6. Personalized Preventive Care
The sixth pillar is individual relevance. Post-screening analysis must translate clinical data into plain-language, personalized insights that the individual can understand and act on. A report that lists values without context does not change behavior. A report that highlights what a specific reading means for that individual, recommends specific next steps, and flags what requires urgent attention does. This is the difference between data delivery and genuine preventive care.
7. Sustainable Business Models
The seventh pillar is financial viability at scale. Preventive healthcare infrastructure must be deployable within a business model that organizations and governments can sustain long-term. For enterprises, this means purchasing infrastructure as a long-term asset that delivers compounding return through reduced medical costs, lower absenteeism, and better workforce intelligence. For governments, it means procurement frameworks that treat screening infrastructure as public health capital investment, not a one-time expense.
How Should Organizations and Governments Build Preventive Health Infrastructure That Scales?
Building preventive health infrastructure that scales requires a deliberate shift in how organizations and governments think about three things: where screening happens, how data is used, and what the investment model looks like over time.
Stop: What to Move Away From
- Stop treating preventive care as a single-site amenity. A health lounge at headquarters does not serve a distributed workforce. It serves the employees who happen to sit near it.
- Stop accepting data fragmentation. Health data that lives in separate systems across separate locations is not an intelligence asset. It is a liability that prevents informed decision-making.
- Stop scaling cost linearly. Every new location should not require a full replication of infrastructure investment. The model must separate screening capacity from fixed cost.
Start: What to Build Toward
- Start deploying screening infrastructure to every location where your workforce or population exists. Uniform access is not an aspiration. It is a baseline requirement for any preventive healthcare strategy that intends to generate real outcomes.
- Start treating health data as a strategic asset. Real-time, standardized, centralized health intelligence across your organization or population is the foundation of every informed decision you will make about resource allocation, risk management, and workforce wellbeing.
- Start investing in infrastructure that compounds. A deployable, AI-powered screening unit generates return from day one and adds to your health intelligence layer with every session. Unlike a fixed health lounge vs health screening robot comparison, where one model hits a ceiling, the robotic model scales without proportional cost increase.
For governments, the transition framework adds one more dimension: procurement as population health investment. Every unit deployed is not just a screening device. It is a node in a national health intelligence network that generates the real-time data governments need to allocate resources, detect outbreaks early, and measure the impact of public health programs within days rather than years.
The organizations and governments that build this infrastructure now will not just screen more people. They will understand their populations and workforces in a way that no legacy system can match, and they will act on that understanding before conditions become crises.

Conclusion
The future of preventive healthcare infrastructure is not coming. It is already here for the organizations and governments willing to build it. Deployable, AI-powered, data-generating screening infrastructure is what separates a preventive care strategy that scales from one that stalls at the first new location. At Kody Technolab, we built Medigo to be that infrastructure, purpose-engineered for the organizations and governments ready to make early detection a structural capability, not a scheduled event.
Frequently Asked Questions
What is preventive healthcare infrastructure?
Preventive healthcare infrastructure is the system of tools, technologies, facilities, and data platforms that enable early detection and intervention before health conditions become serious. It includes everything from physical screening units and digital health records to AI diagnostics and telemedicine systems. Future-ready preventive healthcare infrastructure is deployable, automated, and data-generating rather than fixed, staff-dependent, and episodic.
Why is the future of preventive healthcare moving toward automation?
The future of preventive healthcare is moving toward automation because the legacy model cannot scale. Staff-dependent, appointment-based, single-location screening cannot reach a distributed workforce, a rural population, or the billions of people in developing economies who have no access to early detection today. Automated health screening infrastructure removes every operational constraint that limits scale, delivering consistent, high-accuracy screening at any location without requiring a trained operator on duty.
What does digital preventive healthcare infrastructure look like in practice?
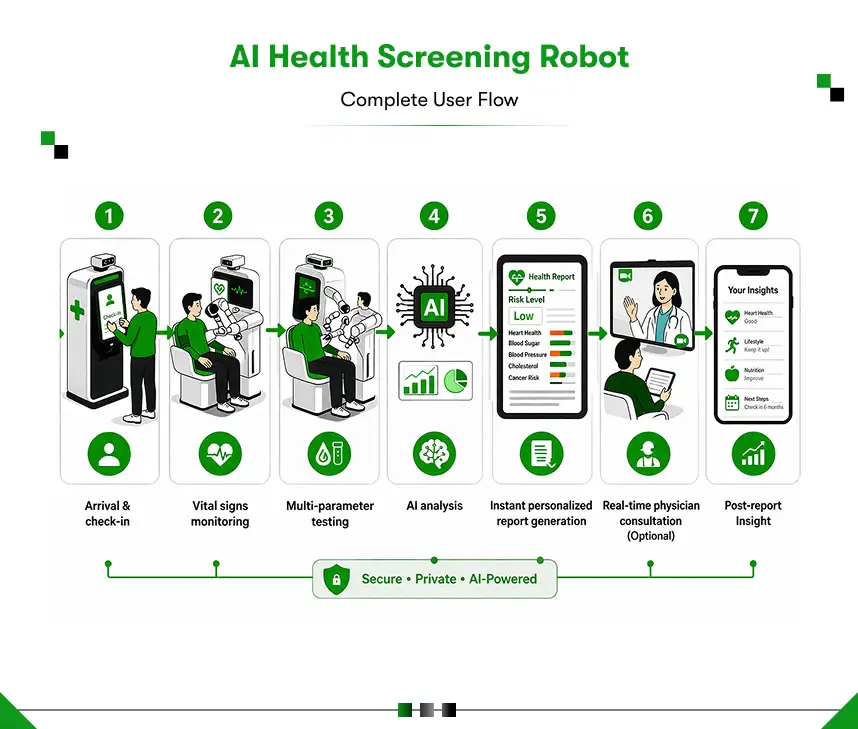
Digital preventive healthcare infrastructure combines autonomous screening units, AI-powered diagnostics, real-time cloud data platforms, and integrated telemedicine into a single, connected system. In practice, it means a person walks up to a screening unit at their workplace, airport, or community center, completes a comprehensive health assessment in minutes, receives an instant personalized report, and connects with a physician on the spot if needed. All data feeds into a centralized dashboard that the organization or government accesses in real time.
How does AI improve the accuracy and scale of preventive health screening?
AI improves preventive health screening in three ways. First, it adapts the screening protocol in real time based on individual responses and demographics, ensuring each session is relevant to the specific person being screened. Second, it interprets results against large-scale validated clinical datasets, delivering accuracy levels that match or exceed manual interpretation for the conditions being screened. Third, it identifies patterns and anomalies across population-level data that no human reviewer could detect at scale, enabling predictive public health intelligence.
What is the most scalable model for preventive healthcare infrastructure today?
The most scalable model for preventive healthcare infrastructure today is a fleet of AI-powered autonomous health screening robots deployed across multiple locations within a single organizational or government framework. Each unit operates independently, screens comprehensively without staff, delivers instant results, and feeds all data into a unified centralized dashboard. The model scales without replicating fixed infrastructure costs, reaches any location regardless of existing healthcare facilities, and generates real-time intelligence that compounds in value with every screening conducted.












 Contact Information
Contact Information