Quick Summary: Healthcare organizations use computer vision to improve diagnostic accuracy, reduce operational inefficiencies, and strengthen patient care delivery. The guide explores high-impact computer vision use cases in healthcare, covering ROI potential, implementation considerations, and operational value across safer, faster, and more data-driven healthcare environments.
Computer vision is changing how healthcare providers process and interpret visual medical data at scale. Today, computer vision use cases in healthcare support radiology analysis, patient monitoring, surgical navigation, medication tracking, and administrative workflow automation with greater speed and consistency than traditional manual processes.
Researchers at Stanford University reported that AI-driven image-recognition technology performed as well as dermatologists in a study that covered the detection of some skin cancers. The study is a clear example of what computer vision use cases in healthcare do. Healthcare systems are also facing a growing challenge of handling more patients, providing preventive healthcare, and data complexity. So, hospitals are turning to computer vision solutions to address these challenges and facilitate quicker clinical decisions.
From detecting abnormalities in scans to monitoring patient movement in real time, computer vision is becoming a practical tool across modern healthcare environments.
The question is, are you moving fast enough to protect your patients, your team, and your business?
What Is Computer Vision in Healthcare?
Computer vision in healthcare is the use of AI systems that process visual data scans, images, videos, and camera feeds to detect, analyze, and act on medical information faster and more accurately than human review alone.
In simple terms, a computer vision system works like this:
- A camera, scanner, or medical device captures an image or video.
- The system preprocesses that image to clean and standardize the visual data.
- An AI model, trained on millions of medical images, analyzes the input for patterns, anomalies, or specific features.
- The system delivers an output, a diagnosis flag, an alert, a recommendation, or a report.
The models powering these systems rely on deep learning and convolutional neural networks (CNNs). These networks learn from enormous datasets of labeled medical images. Over time, they get exceptionally good at spotting what human eyes can miss: a 2mm tumor and early-stage retinal damage.
For hospitals, computer vision reduces diagnostic delays and clinical errors. For insurers, the technology cuts liability exposure and claim costs. To health-tech startups, it creates scalable, defensible product lines with proven clinical value. It reflects real adoption across radiology departments, surgical suites, ICUs, and outpatient clinics worldwide.
Why Executives Are Investing in Computer Vision Applications in Healthcare
Healthcare leaders across the world are not investing in computer vision because it sounds impressive in board meetings, leaders can see the opportunity. They are investing because the numbers behind inaction are far worse than the cost of adoption.
Faster and More Accurate Diagnostics
Computer vision systems help healthcare providers analyze X-rays, CT scans, MRIs, and pathology slides faster and with greater consistency. These tools support early disease detection, reduce diagnostic delays, and help clinicians prioritize urgent cases more efficiently.
- Faster medical image analysis
- Reduced diagnostic workload
- Improved detection accuracy
Operational Efficiency and Cost Reduction
One of the biggest computer vision use cases in healthcare is operational automation. Hospitals use AI-powered monitoring systems to improve patient flow, track bed occupancy, reduce wait times, and automate repetitive workflows across departments.
- Better resource utilization
- Reduced operational inefficiencies
- Lower administrative overhead
Improving Patient Safety
Healthcare organizations also use computer vision to strengthen patient safety and compliance monitoring. Real-time visual monitoring helps staff identify risks faster and respond more effectively to critical situations.
- Fall detection and prevention
- Hygiene and PPE compliance monitoring
- Faster emergency response and incident detection
The ROI case for computer vision is built on four pillars:
| ROI Driver | What It Means for Your Business |
| Reduced Operational Costs | Fewer manual reviews, faster workflows, lower overhead |
| Faster Diagnostics | Reduced time-to-treatment, higher patient throughput |
| Improved Patient Outcomes | Better accuracy, earlier detection, fewer complications |
| Risk Mitigation | Lower malpractice exposure, stronger compliance audit trails |
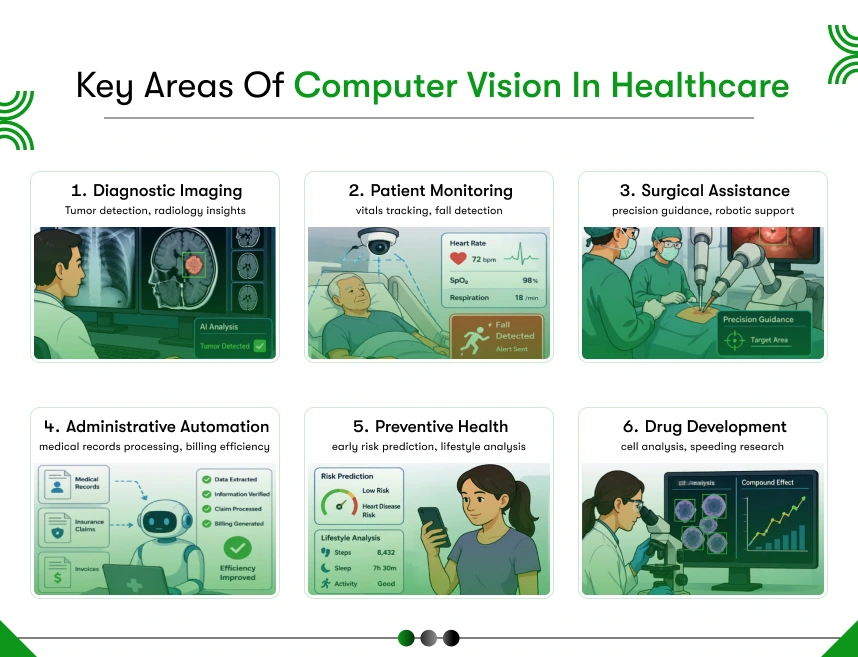
What Are the Top Computer Vision Use Cases in Healthcare?
Computer vision in healthcare covers eight core application areas from radiology and surgical robotics to infection control and remote care, each delivering measurable ROI for hospitals, insurers, and health-tech companies.
Here is a detailed breakdown of each use case and the business impact each one drives.

1. Medical Imaging and Diagnosis (Radiology and Oncology)
Medical imaging is the most mature and widely adopted computer vision application in healthcare today.
Computer vision models have demonstrated up to 95% accuracy in detecting lung cancer in CT scans, outperforming traditional diagnostic methods. AI systems analyze X-rays, MRIs, and CT scans at speeds no human radiologist can match. The system flags anomalies, ranks them by severity, and surfaces the highest-risk cases first.
UC San Diego Health used computer vision AI to prioritize high-risk radiology exams, helping identify a heart failure patient with undiagnosed COVID-19 pneumonia earlier, leading to treatment before the patient needed critical care.
AI-powered computer-aided detection systems can analyze large volumes of imaging data with high accuracy, reducing the time required for diagnosis from days to minutes.
What this means for your business:
- Reduced diagnostic error rates by 30 to 40 percent in comparable institutions
- Faster turnaround on radiology reports
- Lower malpractice exposure from delayed diagnosis claims
- Higher radiologist productivity without additional headcount
2. Surgical Assistance and Robotics
AI-guided surgical systems give surgeons real-time visual support during procedures. These systems do not replace surgeons. They enhance precision, reduce risk, and generate data that improves future outcomes.
The Da Vinci 5 robotic platform offers 8K vision that reveals microscopic nerve bundles invisible to traditional cameras. Real-time overlays highlight critical structures like vessels and nerves, creating digital “no-go zones” during operations. Depth-sensing cameras map tissue layers as procedures progress, updating surgical plans on the fly.
Stanford Medicine implemented computer vision models in surgical settings by integrating augmented reality for real-time visual data analysis, overlaying medical image interpretation on the surgical field to enable surgeons to navigate with greater precision.
What this means for your business:
- Fewer intraoperative complications
- Shorter patient recovery times
- Reduced post-surgical readmission rates
- Stronger surgical training programs backed by video-based AI skill assessment

3. Patient Monitoring and Fall Detection
Hospitals cannot place a nurse beside every patient around the clock. Computer vision fills that gap with AI-powered camera systems that monitor patients continuously, detect anomalies, and send automated alerts to clinical staff.
Computer vision AI helps improve patient monitoring and reduces preventable falls, which, according to the Centers for Disease Control and Prevention, annually cost the US healthcare system up to $50 billion.
Systems like Artisight’s Patient Room solution send automated alerts when a patient attempts to leave their bed. In ICUs, the technology tracks vital signs without physical contact, monitors movement patterns, and detects signs of clinical deterioration before they become emergencies.
What this means for your business:
- Reduced hospital liability from fall-related incidents
- Lower nursing workload through automated monitoring
- Faster response times for at-risk patients
- Better outcomes in elderly care and post-surgical recovery units
4. Automated Health Screening and Triage
High-volume healthcare settings, such as emergency departments, public health checkpoints, and outpatient clinics, struggle with patient intake speed and accuracy. Computer vision automates this process at scale.
Thermal cameras enriched with AI algorithms detect fevers in real time, providing a valuable tool for managing public health risks in crowded areas. Facial recognition systems also assist with rapid patient identification.
AI-powered health screening robots can assess visible symptoms, run initial triage evaluations, and route patients to the appropriate care level, all before a human clinician steps in. This reduces wait times, eases administrative burden, and catches high-risk cases faster.
What this means for your business:
- Faster patient processing at intake
- Reduced administrative staffing costs
- Better early identification of critical cases in emergency settings
- Improved patient experience and facility throughput
5. Drug Development and Clinical Trials
Pharmaceutical companies and research institutions use computer vision to accelerate the drug discovery and clinical validation process. AI analyzes microscopy images, cell cultures, and tissue samples at speeds and scales no human team can match.
Computer vision enables automated interpretation of images to support researchers, with explainable models allowing scientists to identify potential errors and biases in their systems, including patterns in how specific image types are misinterpreted.
AI-based image analysis shortens trial cycles by automating repetitive visual review tasks. The technology also improves consistency across trial sites, reducing the variability that slows regulatory approval.
What this means for your business:
- Lower R&D costs through automation of image-heavy review tasks
- Faster time-to-trial completion
- More consistent data across multi-site trials
- Stronger regulatory submissions backed by AI-generated audit trails
6. Hospital Workflow Optimization
Computer vision not only supports clinical decision-making. The technology also improves the operational systems that keep hospitals running efficiently.
Cross-domain applications of computer vision cover environmental hazard detection in hospital settings and clinical facility monitoring, including patient flow tracking and staff compliance monitoring.
AI camera systems track patient movement through departments, identify bottlenecks in bed allocation and discharge processes, monitor equipment usage, and flag resource gaps in real time. Operating rooms equipped with computer vision generate data that drives waste reduction and quality improvement.
What this means for your business:
- Increased patient throughput without adding physical capacity
- Better utilization of surgical suites and diagnostic equipment
- Lower operational waste across departments
- Data-driven decision-making for hospital administrators
7. Remote Care and Telemedicine Enhancements
Telehealth adoption surged dramatically after 2020 and continues to grow across the world. Computer vision makes remote consultations significantly more clinically useful.
Computer vision monitors facial expressions, eye movements, and motor coordination parameters that are vital for diagnosing conditions such as autism, Alzheimer’s disease, and Parkinson’s disease.
AI systems analyze visible symptoms through standard video cameras during remote consultations. Clinicians receive real-time visual analysis support, helping them catch what a quick video call alone might miss.
What this means for your business:
- Expanded clinical reach without additional infrastructure
- Better diagnostic accuracy in telehealth consultations
- Higher patient satisfaction through faster, more confident diagnoses
- Lower cost-per-consultation for health-tech platforms
8. Infection Control and Hygiene Monitoring
Hospital-acquired infections are one of the most costly and preventable problems in healthcare. Hospital-acquired infections alone cost the US healthcare system between $35.7 and $45 billion annually.
Computer vision monitors staff compliance with PPE protocols, tracks hand hygiene behavior, and inspects patient rooms and high-touch surfaces for contamination risks. These systems run continuously and generate compliance data that supports regulatory reporting.
Computer vision allows automated analysis of patient rooms and surfaces, helping detect dirt, dust, and other forms of contamination that could be harmful to patients and staff.
What this means for your business:
- Reduced infection rates and associated treatment costs
- Lower regulatory penalty risk
- Stronger HIPAA and Joint Commission compliance documentation
- Better patient safety scores that affect hospital ratings and funding
Real-World Examples of Computer Vision in the Healthcare Industry
Seeing how other institutions have applied these systems makes the ROI argument concrete.
Case 1: AI Radiology in a US Academic Medical Center
UC San Diego Health implemented computer vision AI in its radiology department to help prioritize high-risk exams. The system identifies patients who may have suffered undiagnosed strokes and surfaces those cases at the top of the radiologist’s work list, enabling faster intervention.
Case 2: Smart ICU Monitoring
Artisight’s smart hospital platform streams video and audio feeds from operating rooms and patient rooms to a control center. Computer vision algorithms then run on those feeds to capture data across use cases ranging from operational efficiency and waste reduction to patient safety and quality improvement.
Case 3: AI Screening Robots
Thermal cameras powered by AI algorithms detect fevers in real time across high-traffic public health environments. These systems support faster triage decisions in settings like airports, clinics, and emergency departments.
Case 4: Surgical Blood Loss Measurement
Gauss Surgical’s Triton system uses computer vision to scan surgical sponges and calculate exact blood volume in real time during operations. This replaces manual estimation, one of the most error-prone steps in surgical monitoring, with precise, AI-generated data that supports faster clinical decisions.
Key takeaway: Every one of these implementations produced measurable improvements in patient outcomes, clinical speed, and operational costs. None of them required replacing clinical staff, as all of them made existing staff more effective.
What Is the Business Impact and ROI of Computer Vision in Healthcare?
Computer vision in healthcare generates ROI across three categories: cost reduction, revenue and efficiency gains, and risk mitigation. Most institutions see all three simultaneously.
Cost Reduction Opportunities
- Fewer diagnostic errors mean fewer malpractice claims. The average malpractice settlement in the US runs around $420,000 per claim. Reducing even a handful of claims per year recovers significant capital.
- Automated image analysis reduces dependence on manual radiologist reviews for routine scans, freeing specialists for complex cases.
- Continuous patient monitoring reduces incident-related costs, including fall investigations, additional treatments, and extended stays.
Revenue and Efficiency Gains
- Faster diagnostic workflows increase patient throughput per department per day.
- AI-assisted triage routes patients correctly the first time, reducing costly downstream corrections.
- Better resource utilization across operating rooms, diagnostic equipment, and nursing staff reduces overhead without cutting capacity.
Risk Reduction and Compliance Benefits
- Computer vision creates documented, auditable decision trails that support HIPAA and GDPR compliance.
- Consistent AI-generated outputs reduce variability between clinicians and departments.
- Regulatory bodies, including the FDA and EMA, now provide validation frameworks for AI-based medical devices, giving institutions a clear compliance pathway.
| Use Case | Business Impact | ROI Type |
| Medical Imaging AI | Faster and more accurate diagnosis | Cost Reduction + Risk Reduction |
| Surgical Robotics | Fewer complications, shorter recovery | Revenue + Risk Reduction |
| Patient Monitoring | Prevents falls and incidents | Risk Reduction |
| Workflow Optimization | Increases operational efficiency | Revenue + Cost Reduction |
| Infection Control | Reduces hospital-acquired infection rates | Cost Reduction + Compliance |
| Drug Development | Accelerates trial cycles | Cost Reduction |
| Remote Care AI | Expands reach, lowers infrastructure cost | Revenue |
| Health Screening | Faster triage, lower staff load | Cost Reduction |
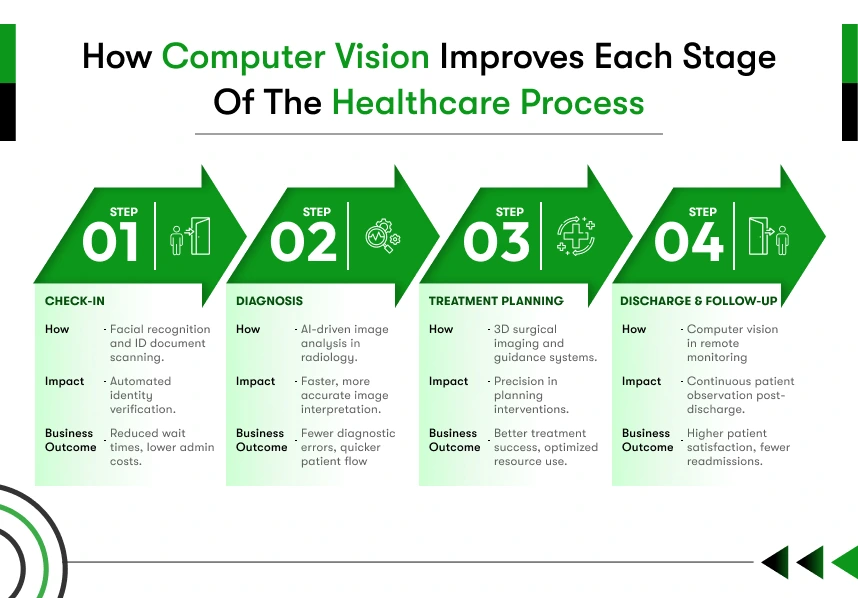
Implementation Roadmap for Computer Vision in Healthcare
Getting computer vision from concept to clinical deployment requires a structured approach. Institutions that skip steps early often face expensive corrections later.
The process follows a clear sequence. First, your team identifies the specific clinical or operational problem the system needs to solve. Vague goals produce vague results. Second, data collection begins under strict HIPAA and GDPR governance, because the quality of your training data determines the quality of your AI outcomes. Third, the right model architecture is selected and trained on your validated dataset. Fourth, the system integrates with existing hospital infrastructure EHR systems, DICOM imaging platforms, and monitoring hardware. Fifth, thorough testing and clinical validation confirm that the system performs accurately across real patient populations. Sixth, deployment begins at scale, with ongoing monitoring and model improvement built into the operational plan.
Step 1: Define the business problem clearly
↓
Step 2: Collect data + establish HIPAA/GDPR compliance
↓
Step 3: Select and train the AI model
↓
Step 4: Integrate with hospital systems (EHR, DICOM, hardware)
↓
Step 5: Test and validate clinically
↓
Step 6: Deploy, monitor, and scale
Partners with deep healthcare domain experience can compress this roadmap significantly. Institutions that try to build these systems without specialized AI expertise typically face 12 to 18 months of avoidable delays.

What Are the Challenges and Risks in Computer Vision Healthcare Projects?
The top challenges in computer vision healthcare projects are data privacy compliance, model accuracy, legacy system integration, upfront costs, and staff adoption.
Every one of these challenges is manageable with the right planning and the right partner. But underestimating any of them creates serious problems.
Data Privacy and Compliance
Medical imaging data is among the most sensitive data your organization holds. Every stage of the AI pipeline, collection, training, storage, and deployment, must comply with HIPAA in the US and GDPR in the UK and EU. Non-compliance carries both legal penalties and reputational damage.
Model Bias and Accuracy
Computer vision is only as reliable as the information that feeds it, so organizations need to prioritize data quality and testing to ensure accuracy. Models trained on non-diverse datasets underperform across certain patient demographics, which creates both clinical and legal risk.
Legacy System Integration
Most hospitals run on systems that were not built with AI in mind. Integrating computer vision into existing EHR platforms, imaging archives, and clinical workflows requires experienced engineering, not just AI expertise.
High Upfront Investment
Computer vision infrastructure hardware, software, compliance frameworks, and integration require meaningful upfront capital. The ROI is strong, but the business case must be built carefully and presented clearly to decision-makers.
Change Management and Staff Adoption
Clinical staff are understandably cautious about AI systems that affect patient care. Effective implementation includes training, transparent communication about what the AI does and does not do, and a rollout plan that builds trust progressively.
How Do You Choose the Right AI Partner for Healthcare Computer Vision?
The right AI partner for a healthcare computer vision project combines proven clinical domain experience, custom development capability, strong compliance knowledge, and a long-term commitment to your success.
Off-the-shelf AI products rarely fit the complexity of healthcare environments. Every hospital has different data structures, different workflows, different regulatory requirements, and different patient populations. A partner that builds custom systems eliminates the gaps that generic products leave behind.
Here is what to look for when evaluating potential AI development partners:
- Healthcare domain experience: Has the team built and deployed AI systems in clinical settings before? Can they demonstrate working knowledge of DICOM, HL7, HIPAA, and GDPR?
- Custom AI development capability: Does the partner build systems tailored to your specific use case, or do they adapt a generic product to fit?
- Compliance depth: Does the team understand the regulatory requirements your deployment must meet, including FDA clearance pathways for AI medical devices?
- Post-deployment support: Will the partner monitor model performance after launch and update the system as your data grows?
- Transparent ROI tracking: Does the partner define measurable success metrics upfront and provide reporting that demonstrates actual business impact?
- Scalability planning: Can the system expand across departments, facilities, or geographies without rebuilding from scratch?
Teams at Kody Technolab Limited work directly with hospitals, health-tech startups, and healthcare enterprises across the world to design, build, and deploy custom computer vision systems that meet these criteria. The team brings deep technical expertise in AI, machine learning, and medical-grade software development alongside a practical understanding of the clinical environments these systems must operate in.
What Are the Future Trends in Computer Vision Applications in Healthcare?
The next phase of computer vision in healthcare moves beyond individual use cases toward fully integrated, AI-driven clinical environments, smart hospitals where every system generates real-time visual intelligence.
Several specific trends are already shaping this direction:
AI and IoT Integration in Smart Hospitals
Computer vision systems increasingly connect with IoT sensors, wearables, and hospital management platforms. The future of computer vision in healthcare is expected to involve AI integration through systems that operate beyond diagnostics for more holistic purposes and care planning. A smart hospital environment generates continuous visual and sensor data that feeds into a unified clinical intelligence layer.
Edge Computing for Real-Time Diagnostics
Cloud-based AI processing introduces latency that is unacceptable in emergency clinical settings. Edge computing moves the AI model closer to the data source, directly onto imaging devices, cameras, and monitoring hardware. The result is real-time analysis without network dependency.
Predictive Healthcare Analytics
Computer vision outputs increasingly feed into predictive models that identify patients at risk of deterioration before clinical signs appear. Early intervention based on AI-generated predictions reduces ICU admissions, shortens hospital stays, and improves survival rates.
Conclusion
Computer vision use cases in healthcare are not experimental anymore. Hospitals, health-tech companies, and insurers across the world are deploying these systems today and seeing measurable results in diagnostic accuracy, operational efficiency, and risk reduction.
Nearly 371,000 deaths happen every year from diagnostic errors. That number does not have to stay where it is. The technology to reduce it exists. What separates institutions that benefit from it and institutions that fall behind is the decision to act and the quality of the partner they choose to act with.
If your organization is ready to explore what custom computer vision can do for your specific clinical and business environment, the team at Kody Technolab Limited is ready to help you build it right.
FAQ
What are the most common computer vision use cases in healthcare today?
The most common computer vision use cases in healthcare are medical imaging analysis, surgical assistance, patient fall detection, infection control monitoring, and automated health screening. Hospitals worldwide actively use these systems to reduce diagnostic errors and lower operational costs.
What are real-world examples of computer vision in the healthcare industry?
Real-world examples of computer vision in the healthcare industry include UC San Diego Health using AI to prioritize high-risk radiology scans, Gauss Surgical’s Triton system measuring blood loss during operations, and Artisight’s smart camera platform monitoring ICU patients around the clock for early signs of deterioration.
How do computer vision applications in healthcare reduce malpractice risk?
Computer vision applications in healthcare reduce malpractice risk by catching diagnostic errors that human reviewers miss, creating documented AI-generated audit trails, and flagging high-risk cases before they escalate. Institutions using these systems report diagnostic error reductions of 30 to 40 percent, which directly lowers legal exposure.
Are there proven computer vision in healthcare examples that show financial ROI?
Yes. Proven computer vision in healthcare examples show ROI through reduced malpractice settlement costs, lower staffing overhead from automated monitoring, faster patient throughput, and fewer hospital-acquired infections. The US healthcare system loses between $35.7 and $45 billion annually to hospital-acquired infections alone, a cost AI-powered hygiene monitoring directly targets.
What should businesses evaluate before investing in computer vision applications in healthcare?
Before investing in computer vision applications in healthcare, businesses should evaluate data privacy compliance readiness, existing system integration requirements, model training data quality, upfront infrastructure costs, and the clinical domain experience of their chosen AI development partner. Skipping any of these steps creates costly delays and compliance risks after deployment.












 Contact Information
Contact Information