As per Statista, the global health market will hit $190 billion by 2025, which opens a vast market for budding and giant players.
Digital transformation has devastatingly impacted many sectors, and the insurance app economy isn’t immune. Winners in the global digital arena are the ones who paddled their wagons with technology. The health sector has pulled in numerous trends, technologies and advanced strategies to reshape their customer experience in a personalized and centric way. Health Insurance App development is one of them.
Gone are the stereotypical approaches of giving discounts and popping their feeds with new policies. Technology like AI, predictive analytics, and RPM allows us to explore new dimensions and better serve customers. In Insurance, the grass is greener on the other side, if you would explore. Embracing these technological advancements and innovative approaches, insurers found better sustainable ways to serve customers and stay competitive.
Intrigued? Let’s delve into and unfold some aspects of this unprecedented shift in the dynamics of health insurance apps.
Health Insurance Apps Market Overview
In the United States, the health and medical Insurance market is soaring faster with substantial growth rates, and it is expected to catch a faster pace significantly in upcoming years. The Health Insurance industry comprises multiple carriers – private and public health, medical and dental Insurance, and more.
Each player is building new strategies and fine-tuning their existing ones to stay ahead in a competitive edge and meet the market challenges. Atena, Humana, Cigna, Anthem Inc., and UnitedHealth Group Inc. are a few of the dominant players in the segment that leveraged the latest tech trends. Being tech-savvy, they shifted the lens from transactional roles to relationship-based customer services.
The health insurance explosive growth is coupled with digital health apps, telehealth services, health tracking, data analytics, technological advancements, and much more. Health insurers can expand their operations, achieve better ROI, scale faster, and expand their operations more efficiently by developing a health insurance app.
For example, Oscar leveraged advanced technology, developing the first health insurance app with 1 million active members.
Oscar was the first to bring a Health Insurance app into the industry. Considering convenience and accessibility and grabbing customers where they are accessible, Oscar leveraged technology and was rewarded with 1 million active members.
However, this was not the end. The industry followed the trend, magnetized profits, and converged with its customers with this ecocentric model.
Adapting the trend and following evolution, Aetna, a renowned health insurance company, grabbed 2 million downloads with a whopping 4.8-star rating. Collectively, numerous factors contribute to the growth and sustainability of Aetna.
Now, let’s explore the intricacies of Aetna’s path to success and decipher the elements that have set it apart, earning it the prestigious label of an industry “unicorn.”
What Made Aetna a Health Insurance Giant?
Innovation is key to success! And Atena proved it to be the one. Chameleoning itself as per industry standards and digital shifts, adapted to technological advancements at every step.
- 2010 – Surge in smartphone usage driven Aetna Health Insurance app development and product marketing.
- In the mid-2010s – The adoption of big data and analytics to get better insights about health records and cater services accordingly.
- 2010s and 2020s – Harnessed artificial intelligence, machine learning, and the latest advancements to offer personalized health plans and recommendations.
- Pandemic Era – Integrated virtual healthcare and digital services to give better convenience, accessibility, and services along with their insurance products.
- Post-Pandemic – Atena’s approach turned more user-centric, prioritizing seamless online services, robust data security, and enhanced customer experiences.
Gaining an understanding of the market position compared to peers, Atena strategically made developments and set competitive benchmarks.
Understanding the gaps in the health insurance industry – be it coverage, affordability, faster claim process, mental health coverage, geographic limitation, complexity of plans, etc. Atena started with solution-focused, state-of-the-art features in their Health Insurance App development.
- Some of the unique and standout features of the Atena app are,
- User-friendly interfaces,
- comprehensive coverage information,
- healthcare providers on their radar,
- mobile app accessibility,
- telehealth service integration,
- personalized health plans,
- data security measures,
- wellness programs,
- preventive care focus and incentives, and more.
Data security, wellness programs, and transparent customer support set Aetna’s bar high in the health insurance industry.
Why Develop a Health Insurance App?
The reasons are numerous! Let’s delve into some insights and statistics that underline the significance of developing a health insurance app.
⏩ As per McKinsey, Medical Insurance is the fastest-growing InsurTech segment.
Insurtech is gaining traction and remains a booming segment in the digital landscape. To stay competitive in the digital landscape, you the industry should align and collaborate with the integration of innovative technologies.
⏩ Capturing a 9.50% CAGR, the health insurance market size would hit USD 3.619 trillion by 2028.
Entering the market with cutting-edge advancements, trends, and technology and harnessing resources is key to driving transformative change and better business goals.
⏩ As per Mckinsey, the revenue bagged for private health insurance in the global market is €1.3 trillion and is expected to multiply by 2025.
The demand for healthcare insurance is increasing due to the growing prevalence of chronic disease along with an expanding population. Insurance is the need of the hour.
Focusing on Health Insurance App Development is not just about following trends; it’s about seizing the opportunity and chalking out the financial goals to business goals. Its instrument is to build a profitable business by reducing costs, facilitating sales, and enhancing financial operations.
Benefits of Health Insurance App Development:
- Bridging the gap between insurers and payers.
- Nurturing better relationships between clients and insurers through online services.
- An affordable and user-intuitive platform where users can get all services at their fingertips.
- Choose and understand the insurance plan that works for them.
- Streamlined process to reach out to doctors and hospitals that support their insurance network.
- Get a personalized recommendation plan per their health profile, financial situation, and specific needs.
- To get better data and insights. Insurers can get data, analyze it, and improve services and products.
- Navigating all the services in a user-friendly and accessible way.
A superior health insurance app goes beyond balancing responsiveness and aligning with customer needs. It should meet the touch points of current trends, adapt to a strategic approach, and simultaneously fulfill the goals of customers and businesses.
Let’s unfold the essential features and functionalities that should be on the Health Insurance App Development checklist.
Features and Functionalities to be Integrated in Robust Health Insurance App Development
The app’s anatomy, features, and functionalities represent the app’s heartbeat and intelligence. They must function cohesively and optimally to maintain the app’s vitality. However, every business’s needs and goals are different; a custom health insurance app is a solution to manage everything and sync with business goals.
User Profile Management
User Profile Management helps accumulate essential information from the user to set up a profile on the app, from insurance ID cards to policy details, nominees, and other information. This would facilitate users to access and get their health insurance ID cards digitally and manage on-the-go. While for insurers it would make it easier to understand insights, comorbid conditions, data, and more to facilitate services efficiently.
The idea was integrated into Health Insurance App Development by the United Health Care app to reduce administrative work, reduce errors, get real-time updates, better customer engagement, and cost savings.
Dashboard
A dashboard offers a 360-degree view of a health insurance app. It consolidates all crucial information, including coverage details, claim filing, premium payments, health monitoring, retention rate, performance metrics, etc. It helps companies to make informed decisions based on real-time data. Dashboards streamline processes to manage coverage, claims, and personalized interactions.
Technology-driven giants United, Atena, Humana, and Oscar Health employed data-rich analytical dashboards to drive improved care coordination and better customer satisfaction.
Health Insurance Plans and Listings
As per Forbes Advisor, 18% of consumers do not have a health insurance plan as they cannot find a plan that meets their needs.
Simplicity and customer focus are paramount. Whether it’s health insurance plans or listings, clarity trumps. A user doesn’t want to find a needle in a haystack. Instead of jargon and perplexing things, presenting information in easy-to-understandable tables is key to grabbing more customer attention and retention. Customers get access to coverage, benefits, pricing, and everything at a glance.
This would encourage them to make better decisions, and for insurers, it would help them understand customers’ insights.
Search in-network hospitals or doctors.
Convenience and accessibility are magnets to attract customers. At times of urgent medical needs, an immediate instinct and option is to use digital devices to find nearby facilities. A Health Insurance App development should be able to provide in-network doctors, hospitals, and clinics covered by their insurance plans.
This would encourage customers to increase usage of apps, engagement, better-claiming process, and cost control. At the same time, insurers would get data insights, avoid fraud, and stay connected with customers in their peaks and valleys.
Remote Patient Monitoring
Remote Patient Monitoring is rising, and it’s a win-win for insurers and consumers. With the surge in telehealth usage, insurers accumulated benefits of improved quality of care, understanding of patients’ health conditions, fewer trips to the hospital, better access to healthcare, and more holistic insights.
Better insights help insurers make data-driven decision-making, more accurate underwriting, risk management, fraud reduction, and improved outcomes. RPM is a game-changer tool that benefits everyone in the healthcare ecosystem. For example, Atena RPM resulted in better management of chronic conditions, reduced healthcare costs, and enhanced patient adherence.
Health Record Integration
Incorporating electronic health record integrations gives you a comprehensive overview and management of customer health data. This centralized system would entail medical history, medications, and doctor details and enhance claim procedures. Overall, this would help insurers craft personalized policies, sustainable products, or services.
Claim Processing
As AI matures, insurers leverage the technology to improve customer relationships through better and easier claim processing.
The speed of settlement has reversed discontent and dissatisfied customers with improved claim processes. Many of the claims required hefty and tedious repetitive tasks. Tandem with predictive analytics, AI, and Big Data, the claim process is streamlined, yields efficiency, reduces fraudulent claims, analyses data patterns, and boosts productivity benefits.
As per Forbes, integrating claim process accuracy improves 99.99% operation efficiency and 60% customer experience.
Atena, Humana, Cigna, Oscar Health, United Health Care, and other major players have embraced these features and witnessed significant improvement.
Next is integrating these features and building a Health Insurance App Development.
Essential Steps of Health Insurance App Development
Though health Insurance might seem generic, every business has specific outlining requirements. Our process to build a health insurance app is as follows:
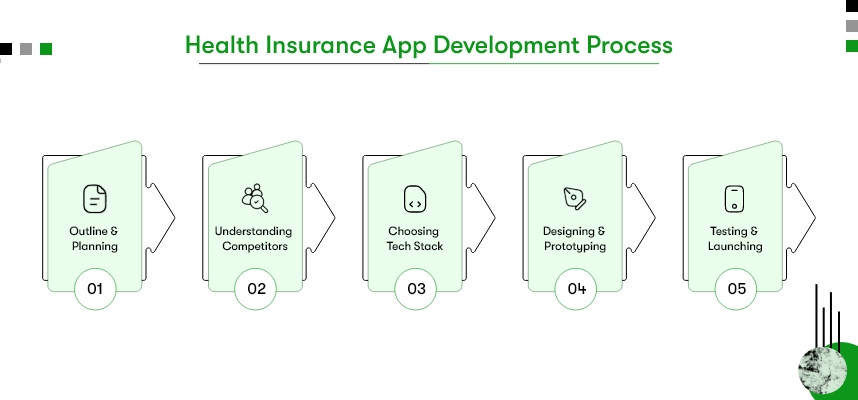
Outlining and Planning
The initial phase includes extracting information, outlining requirements, and understanding the nuance of the projects. Be it audience, goals, purpose, requirement, platform, and everything. It’s about nailing down and setting clear goals to craft apps meticulously.
Understanding Competitors
Whether the business is small or enterprise-grade, we drill down the deets, understanding competitors and chalking out all the details essential. Examining and observing competitors would help understand extensive features and leverage technology and strategies in a single direction to build a top-notch app.
Choosing Tech Stack
The foundation must be strong for an app to be robust and rigid. This includes selecting libraries, languages, frameworks, development toolkits, programming methods, and more to build the high-performing insurance app. Picking the right tech is necessary to sustain the stability, scalability, and security of your health insurance app.
Our geeks can help narrow down choices that comply with your business goals and targeted audiences. Want to build Android and iOS apps simultaneously? Hire expert Flutter developers! Consult with our industry expert to get answers to all your questions.
Designing and Prototyping
The requirement is chalked out; it’s time to lay the foundation by selecting UI/UX and building the codebase. It’s time to shift gears and turn on-paper visionary things into breathing applications through coding.
An agile and expert team on your side would help build a comprehensive app that covers client-side interface, app creation, integration of backend endpoints, and much more.
Flutter or React Native are preferable options for cross-platform apps, while Kotlin or Swift dominate for native ones.
Testing and Launching
Once the app undergoes the stringent testing and bug-fixing process, it’s ready to be launched in the market. Post-release maintenance must be prioritized to sustain an application while making it a successive story.
Regular updates, fixes, upgrades, and additional features, further contribute to the vitality of the insurance app while magnetizing clients.
Game-Changing Technology Trends in Health Insurance App Development
With a ‘digital-first’ sweep in the healthcare landscape, driven by Gen Z, consumers, data, automation, and artificial intelligence, the USD 5 trillion global insurance market is changing its path to redefine business.
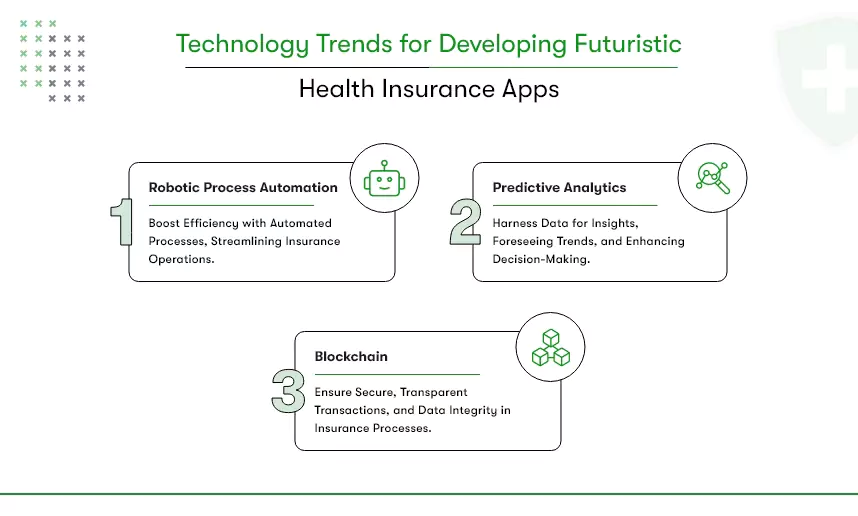
Robotic Process Automation (RPA)
Robotic Process Automation (RPA) in Insurance takes center stage to process faster and minimize fraud. This will eliminate brokers and paperwork, improve customer service, and enhance claim management.
For example, InsurTech giant Lemonade’s business model deploys AI and behavioral behavioral economics that accurately determine risk and help achieve higher profitability.
AI and automation enormously impact profitable outcomes in customer experience, cost optimization, marketing competitiveness, operational efficiencies, and much more.
Predictive analytics and proactiveness
Implementing predictive analytics in insurance ushers opportunities for new growth. Harnessing Tech-enabled data would help you curate personalized premium plans, new approaches, underwriting, claims, and other services that increase productivity and allow for higher-quality customer touchpoints.
In addition to revamping core processes, predictive analysis in the ecosystem is helping to optimize the whole insurance process proactively. Insurers analyze customer behavior and patterns while seeking strategies to minimize expenses and offer the best possible services.
Read Also: Top 10 Game-changing Use Cases of Predictive Analytics in Insurance
Blockchain
Security and safety are integral elements of Insurance. A single leak could endanger the trust and loyalty of customers. Sometimes, these breaches could steer toward criminal activity and civil lawsuits. Integrating advanced technologies like blockchain would help insurance companies manage data more meticulously and consciously.
Blockchain technology is widely adopted to manage and encrypt sensitive customer data. The deployment of blockchain in Insurance would make the process secure.
Blockchain technology safeguards your healthcare solution with a transparent, incorruptible, and decentralized log of medical records. Some examples built on blockchain technology are Medical Chain, Guardtime, Akiri, and more.
How Much Does It Cost to Build a Health Insurance App?
Giving a fixed price tag for Health Insurance App Development won’t be justice, as it undertakes numerous facets, elements, components, and factors. Building an app is a multifaceted process, it encompasses UI design, backend, frontend programming, API integration, testing, and ongoing maintenance. The expenses may rise due to these factors.
The price might fall between $50,000 – $70,000 to give you a ballpark figure.
| Complexity of App | Average Duration | Cost Range |
| Basic Features App | 3-6 months | $50,000 – $70,000 |
| Medium and More Features Integrated App | 6-9 months | $70,000 – $90,000 |
| Highly Complex (Latest Features and Technologies) App | 10+ months | Cost may vary accordingly |
This table provides a breakdown of health insurance app development costs and timelines based on the complexity of the project and the range of features integrated.
To know more about cost and timeframe, our team is here there to help you.
Revolutionise and Reshape The Health Insurance Industry with Kody’s Tech-Driven Expertise
Innovation is the master of invention. And dynamic health insurance requires top-notch innovative approaches, expert guidance, and cutting-edge technology. At Kody Technolabs, we understand and comply with future-proof strategies and excel in creating various applications. We are backed by happy clientele from healthcare, fintech, insurtech, manufacturing, etc.
Our secret sauce combines technology, expertise, industry trends, and strategic thinking. With an ever-changing healthcare landscape, you must hire dynamic flutter developers to upscale projects. Conceptualise designs and development with our end-to-end services to streamline the deployment and maintenance of your assets solutions.










 Contact Information
Contact Information